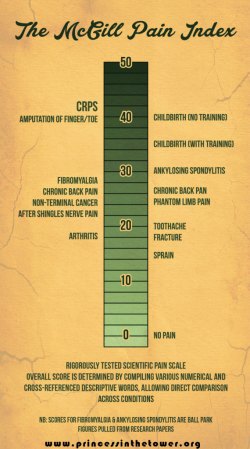
There are so many of us living in the constant pain of CRPS (Complex Regional Pain Syndrome), which sits at the very pinnacle of the McGill Pain Index. There is no way to describe it, I know that I never would have believed such an illness existed, much less believe the sheer ignorance on it by medical professionals despite it’s all-pervading grip on everything in a patient’s life.
It’s frightening. It can be lonely, we are so often isolated but even in company, our invisible symptoms set a window between us and the world. Social media and the internet may have helped us cope, even have some semblance of life from our homes or bed, though sadly even that time can be limited because of the pain caused by it.
Yet though awareness is growing, our CRPS community too, a beautiful and evolving shared courage, so many have never even heard of it even in the medical community and herein is the heart-wretching sadness and danger too, we don’t have to live with this disease. The chance of remission if caught early enough is high. After months of disbelief or confusing symptoms and severe pain, that chance decreases and continues to decrease, making it all the more difficult to come to terms with this ‘new normal’.
CRPS Awareness Month
As I proudly wore orange in honour of CRPS/RSD Awareness Month, I thought on how to raise awareness and of course, help those also living inside a body that CRPS has turned into what can only be described as some kind of medieval torture device. Although this website is dedicated to helping everyone who lives with pain and painful chronic illness, CRPS is the excruciating inner gremlin that snatched the rug from under my 22-year-old feet, before all else, and it being the month of spreading awareness, this post focuses on ways you can help yourself as a patient.
If you have recently been diagnosed with CRPS, this piece by friend and CRPS warrior, Lili at Taming the Beast: So You’ve Been Diagnosed with CRPS, What Now?
Everyone with CRPS needs good medical support and treatment. While this is not always possible, with both knowledge and awareness of CRPS being so sparse, especially if you live in a rural or remote area, and the great difficulty in its management and treatment, this website can help guide you in things that help improve your pain and function.
How is Complex Regional Pain Syndrome treated?
As pain involves the whole person and because CRPS is so much more than ‘just’ pain, to get the best outcomes for you and your symptoms, treatments and management usually require a combination of the following approaches:
- Pacing and planning everything. Unless you use pacing and plan, you may find that you manage for a while but the painful payback of exceeding limitations is fierce. Visit the page on pacing here.
- Relaxation techniques: diaphragmatic breathing, meditation, body scan, restorative/therapeutic yoga.
- Mindfulness has helped a lot of pain patients cope but distraction also is a useful coping/pain management tool.
- Meditation and other forms of relaxation – vital to calm your sympathetic nervous system.
- Gentle movement and mobilisation techniques: aqua physio, Tai Chi, Chi Kung (seated or standing), restorative/therapeutic yoga.
- Learning and practicing every coping and pain managing technique that helps you.
- Brain training techniques – so much of the focus in treatment has shifted to retraining your brain to counter and in theory reduce the maladaptive neuroplasticity that CRPS causes.
- Use of pain medicines and medical procedures.
- Complimentary medicine also visit this wonderful site, written by CRPS warrior, friend and complimentary therapies expert.
Successful treatment of RSD/CRPS is dependent on:
- Early diagnosis. If diagnosed early, the prognosis is very good.
- Begin treatment of the RSD/CRPS process. The key approach is to provide enough pain relief in order to undertake rehabilitation, though it is obviously still going to be painful (slight understatement!). However in spite of this being a very reasonable goal, it is sadly so frequently not met, with thousands of CRPS patients being under-treated and facing far greater challenges than they already do.
- The primary aim is to restore function. This is crucial in increasing and maintaining mobility but must be paced and the increase in movements very gentle, very slowly (to avoid flaring-up), and inside your personal limitations. To read more on this, visit the page on Pain Pacing here.
- Movement is vital. If you do not move, even if it is as humble as wiggling your toes regularly, your muscles will weaken, causing further problems and pain, and the body, which is designed to move, is at greater risk for other complications. Many patients find that exercises in warm water are far less painful. The water itself is soothing, supportive and also has the added benefit of reducing allodynia, which is the pain caused by innocuous stimuli.
- If newly diagnosed, it is vital to control pain so that pain pathways in the brain do not become maladaptively rewired, making recovery even more difficult. The process by which pain becomes chronic is only hampered by excessive stimulation of your CNS so do everything you can to be proactive, no matter how seemingly impossible, not to mention excruciating the rehabilitation process is.
- Techniques to calm your SNS (sympathetic nervous system) become vital, as does having a basic knowledge of brain retraining techniques. Though I will expand more on this in a separate post.
Stimulus = Pain
The brain behaves a little like a faulty and hyperactive car alarm in CRPS, thinking that everything is dangerous, in turn sending its vicious pain signals at the most innocuous of stimuli. Sound, vibration, even a breeze can send our pain levels soaring so ensuring that your environment is as calm and quiet as possible has a huge effect on your levels of pain and other ANS symptoms.
This is of course ever so hard to convey to healthy people, who have a tendency to think they know best or that “it can’t be that bad,” but it is. The perplexing symptoms of CRPS are incredibly real to us and without the luxury of denial, unless we are allowed the space and grace for our over-stimulated systems to calm and settle a little, it becomes hard simply interacting with others who do not grant you the quiet and non-stimulating environment you need to manage your CRPS.
With central sensitisation being an added cause of increased pain, allodynia and hyperalgesia, limiting stimulus becomes a vital part of coping and managing your pain levels. Using an eye-mask, listening to the ocean waves or brainwaves can be soothing too, can help you calm your over active sympathetic nervous system.
Retraining the Brain
In healthy bodies there is mental map of where the body is in space and this allows us to function without having to check where we put our hand to pick up a glass or which is the left or right hand. This ability can be lost in CRPS and this altered function seems to be part of the reason that pain persists in CRPS. The Graded Motor Imagery program helps you to re-train the recognition of where the body is in space. For more information about GMI, also an app that you can use to train on your mobile (cell) phone, even from your bed, visit the GMI website here.
GMI and Mirror Therapy
Mirror therapy can help in the early stages of CRPS. This procedure aims to “teach” the brain that the limb where pain is being felt is actually OK, that is, not dangerous or cause for alarm. In CRPS normal inputs such as touch, stroking and movement are misinterpreted as painful.
This ongoing “painful” interpretation is a big part of the problem. With the brain perceiving everything is dangerous, even the most innocuous of stimuli causes and exacerbates our pain.
With mirror therapy, a potent part of GMI, a mirror is set up between the limbs so that the affected one is hidden, but the mirror image of the unaffected limb looks like the one that is in such intense pain. Both limbs are moved gently but the CRPS one is hidden and the brain “sees” what looks like the painful limb working, without pain, and in turn “learns” that it can be moved without harm, see mirror therapy for more information.
Graded Motor Imagery is showing great promise, even in long-term cases of CRPS. Do be aware that it can momentarily increase the pain in some patients but that this evolves into lower pain levels and increased function. GMI helps you to re-train the brain to behave more normally, less reactively, and this has been found to help decrease pain and improve mobility.
Mirrors may be used for a variety of pain and disabilities but especially involving the hands and feet, with many patients, including CRPS warriors and angels, gaining pain-relief and improved movement by using a mirror. Be warned that it can worsen before improving.
What else could I do at home?
- For GMI, you could browse through the internet or a magazine and look at pictures of hands and feet and work out which is right and left.
- Imagining movements or your CRPS limb by using certain postures or positions – Imagery is a great way of ‘exercising’ the mind/brain using a progressive approach. This approach reduces the chance of pain flares and helps you make better progress.
- De-sensitise your CRPS-affected limb(s)/areas by using a flannel in the bath; gently move it over the area and keep affirming that “this is just a soft flannel” – although the research is yet to conclude on this, it has had positive reports of it helping patients.
Mobilisation, Gentle Movement and Mindful Exercise
Physical therapy to maintain flexibility, strength, and range of motion is important but find out your pacing limitations for each activity and build up very slowly to avoid and set-back or falre-up, and never exceed those limitations. Not using an affected limb can result in atrophy and eventually not being able to use the limb.
It’s crucial to undertake rehabilitation, though it is obviously painful, unless restoring function can occur, the CRPS can worsen. I understand. It’s excruciating. The last thing you want to do is move. It can feel like walking on burning broken glass when you have CRPS/RSD in your foot/feet, or burning-iced limbs, no one would move with that. But the vital thing to consider, and the thing I want you to avoid at all costs, is to not move at all as this will worsen everything.
It’s a delicate and difficult balance of moving enough but not moving too much. There are and will be times when you flare and are stuck but during rehabilitation, take it very slowly. In those early stages and months of CRPS, even wiggling your toes or fingers (depending on where it is or begins) is excruciating yet it can be the start of your rehabilitation and increasing your mobility again. So wiggle those toes.
With thousands of CRPS patients being under-treated and facing far greater challenges than they already do, so many do not receive adequate treatment. Another thing that helps me personally and something I will expand on in a post of its own is baths and exercises that you can do – very gentle exercises – I tend to call it mindful movement as exercise conjures up the wrong image.
If you do not move, your muscles will weaken, causing further problems and pain. For pain relief, to reduce stiffness, increase circulation, ease movement and regain a good sense of your body are all important in maintenance and rehabilitation but also if you need to spend a long time in bed or resting due to high pain levels, see Pain-Relief and Coping for Severe Pain.

To mobilise tight & stiff body regions and develop control of movement; gradually progress from just a couple of repetitions (see a physical therapist for guidance on how to strengthen muscles and rehabilitate). Progressively build up your tolerance slowly, this is vital. To begin you may only do two repetitions of an exercise and that is fine. Consistent and slow is far better than pushing through and causing a flare and therefore set-back in progress.
Always keep within your limitations, increasing your timed activity very gradually. For example, tai chi can be done in a chair, also see this seated tai chi routine here; restorative or therapeutic yoga is incredibly gentle or even mindful and gentle movements in the bath can help reduce your pain and increase muscle mass and strength.
Swimming/aqua physio is also immensely helpful with RSD/CRPS. Also read: 3 Natural Ways to Reduce and Manage Your Pain and see Natural Therapies to Ease Chronic Pain.
Graded Exposure & Pacing
There are often particular activities that are challenging, painful and sometimes avoided for fear of causing damage or harm. You can use pacing to gradually re-engage with some of these activities. Pacing means that you set a baseline and work towards your goals, see the Pain Management page for more information. You may also enjoy this useful piece that shows you how to desensitise using epsom salts and bathing.
Mindfulness & focused attention training
Mindfulness can have profound ways on your relationship with your pain. Also as a way of reducing the emotional aspects of pain. Mindfulness helps us to respond skilfully to the inevitable physical suffering that comes with being in bodies when we have CRPS/RSD.
Our habitual reaction to physical discomfort is some form of resistance and aversion, leading to increased frustration or anger and therefore increased pain. In practicing mindfulness, the habitual response is replaced with one that’s more skilful.
For example, if we’re suddenly in increased pain, we can let the habitual response of anger or frustration brew and increase, which increases our mental suffering and physical pain too because the muscles surrounding the pain tighten in response to our frustration. Mindfulness offers many other benefits too. Click here for an example of one of the mindfulness techniques.
Brain-Focused Strategies
Modern neuroscience has transformed the entire view of how our brains work and are affected by chronic pain. With new ways of approaching pain though our understanding of the brain in chronic pain, alongside what we now know about the heightened responses of CRPS – which drastically alters the way our body processes pain, as well as function pf the sympathetic nervous system – we can target the adaptations and changes using particular types of sensory and motor training. For example, the graded motor imagery program and tactile discrimination training.
Ways To Train Your Brain
- Visualisation – Increasing research suggests that visualization of an activity and the action of that activity is processed in the same way in the brain. Because your brain knows no difference, this may be a very useful tool in retraining the brain.
- Relaxation (including mindfulness and meditation) – It quiets an overactive brain, which offers your mind an opportunity to refresh, even imagine desired outcomes, such as visualising you walking – a powerful technique because as far as your brain is concerned, the same areas light up as if you were actually walking. Although research is in its infancy, even 5 minutes a day of visualisation can help. It also reduces stress-related brain chemicals and increase nourishing brain chemicals.
- Nutrition and Rest – How well you eat and how much you sleep will positively affect your brain’s ability to function but it’s not always so simple. Read When Pain Interrupts Your Sleep. I will cover more on nutrition and pain in a separate post.
- Psychological techniques – Keeping your mind as at ease as possible is crucial in managing such high levels of constant pain. Read: How to Use Pain Psychology Techniques to Reduce Anxiety, Depression, Anger and Guilty and also see: How to Cope and Heal Depression When You Have Chronic Pain and illness
- Laughter makes your brain increase production of serotonin and dopamine, both neurotransmitters play a massive part in mood and also your pain. Read more here: Why Laughter is the Best Medicine When You Live in Pain.
- Stimulation – Choosing activities that make you feel good, whether active or passive activities, reinforces the neuronal pathways. Novelty and focus (attention) is another big factor in creating and reenforcing neural pathways, and retraining your brain.
- Mindful Movement, as detailed above, is a fantastic way to train your brain.
Imagery & visualisation
Motor imagery is used as part of the graded motor imagery programme and as a stand alone brain focused training. When we think about movement, the same areas of the brain are active as when we actually move. So if we imagine ourselves walking, running, moving in any way at all, the areas of our brain involved in executing those movements, lights up as if we are actually performing them.
Using this physiology within the cortical network allows us to re-train normal movement (how the brain plans and then executes precise and well controlled actions) at the early stages of rehabilitation. Visualisation is a way of changing the body physiology in a positive manner thereby benefiting the physical self, mood and creating a positive context for rehabilitation.
It is also a wonderful way to help you manage the intense pain. Escape wherever you wish to. Put headphones in, listen to calming music or guided meditations, or simply the ocean waves and pretend you are on a hot beach in the sun.
You can do anything or be anything you please in this clandestine world. Imagine you are walking along a wooden pathway by the tropical sea, or through a bluebell-ladden wood. The [inner] world is your oyster.
Living with CRPS is hard. Escaping to paradise, whatever your personal paradise may be, is healing, nurturing. Anything that helps you cope and reduces the pain, both physical and psychological, is crucial. So escape. Give yourself a gift and try visualisation.
Useful Links for Patients
Here are some incredibly useful links. The first is a link to the RSDSA, the second was compiled by friend and fellow CRPS warrior, Elle and the Autognome: CRPS FAQ This comprehensive and regularly updated list is a fantastic resource for both patients and caregivers/loved-ones of patients.
Facebook offers some unparalleled info, support too of course, for patients. In fact, this blog started out as a Facebook page and grew from there. I think all of you should head to a like this instant (no pressure) to: RSD/CRPS Research and Developments, an unbiased research page run by patient and superstar, Sandra. Also, the miracle that is Marie aka Elle and the Autognome has a wonderful page, especially for the dysautomnia info, which is hard to find: Elle and the Auto Gnome (Living with RSD / CRPS & Dysautonomia). Biowizardry combines CRPS info and experience with the wonder that is Isabel, patient and scientist. Taming of the Beast is the Facebook page for the website mentioned above and also a resource for natural healing and alternative health (created by a CRPS warrior/angel).
CRPS UK Clinical Research Network, RSD Hope, Complex Regional Pain Syndrome – New Zealand, International Research Foundation for RSD/CRPS, a.k.a. International Foundation for CRPS & RSD, a.k.a. RSD Foundation, Women in Pain.
Read A Letter to Those Who Do Not Have CRPS/RSD here.

 It would also be a fine time to mention the awareness tee-shirts and other items on the CRPS, Art & Spirit Cafepress shop, which you can purchase directly here. All of the proceeds go straight to the charity, which is involved in sharing information and knowledge with those who need it to help bridge the gap between doctors and patients. If you can’t find what you’re looking for in the shop then let the CRPS, Art & Spirit team know here because they may well be able to rustle up a design at your request.
It would also be a fine time to mention the awareness tee-shirts and other items on the CRPS, Art & Spirit Cafepress shop, which you can purchase directly here. All of the proceeds go straight to the charity, which is involved in sharing information and knowledge with those who need it to help bridge the gap between doctors and patients. If you can’t find what you’re looking for in the shop then let the CRPS, Art & Spirit team know here because they may well be able to rustle up a design at your request.
There is a drive to get information to doctors on the Facebook page CRPS Research and Developments, so pop in online and ask for a postcard or two to drop in for your doctors to read. This is important. So very important. So many lives are lost to CRPS each year, and if we wait for the general medical field to catch up with the specialist research it will be too long. Too late for another soul who found that their safety net was missing because CRPS was not understood.
Natural Therapies and Techniques
Hyperbaric Oxygen therapy had has amazing results with CRPS, even in long-term CRPS and is especially useful as no painful manipulation is applied.
Acupuncture can be helpful at all stages of CRPS, not just for pain but for side-effects from medication and overall well-being. However, it can be difficult to find an acupuncturist who is knowledgeable [or gentle] enough with regard to managing CRPS. Asking for extra fine needles can make a huge difference. Never needle the epicentre of where the CRPS began as it can cause a flare-up of symptoms.
Myofascial Release taken slowly and gently on the body in long-term CRPS (avoiding parts of the body that are too painful, hyperalgesic or allodynic), can be immensely healing body work, especially if you have been bed-bound or sedentary due to your pain, as it can help you recondition your body and lengthen your muscles and fascia.
Using a transcutaneous electrical nerve stimulation machine (TENS) can help confuse the pain signals, thus reducing them and is a helpful aid.
Practicing Mindfulness and meditation can help ease some of the symptoms and help the patient relax, in turn reducing pain.
SCENAR therapy has helped some patients improve their mobility but can be expensive with a therapist. Investing in your own unit can cost from £400 but with each therapist treatment being £40-60, it is comparatively better value.
Effective sympathetic blocks have helped some patients by blocking nerve impulses with anaesthetic agents used in severe pain. Blocks may provide permanent or temporary relief. They do not, however, help once the pain becomes sympathetically independent, which tends to be within the first three years but varies from patient to patient.
Hydrotherapy and aqua therapies can help CRPS patients immensely. See this video for CRPS and aqua physiotherapy:
One particularly healing therapy is Watsu, which not only relieves pain and increases flexibility, it is also incredibly relaxing and calming to the nervous system. Personally, it’s the finest of all therapies in terms of both easing pain, soothing the mind and offering much-needed tranquillity to the spirit. Watch this calming video:
Sign-up and receive a free flare-up toolkit and regular posts and tips on living – and coping – with severe pain and chronic illness ♥
Also see the main page on Complex Regional Pain Syndrome here.
Click here for a free pamphlet on CRPS from the National Health Institute.
[avatar user=”jomalby” size=”thumbnail” link=”www.princessinthetower.org” target=”_blank”] Gentle hugs x[/avatar]








This is a great article. Thank you for your hard work. I have had CRPS/RSD for 13 years. My daughter has had it for 7 years . We were both diagnosed immediately as I am an RN and have had patients with this disease over the years. It has spread to full body with me.
I do take issue with your statement, “The chance of remission if caught early enough is high.” That is an immeasurable statement. I know of only a handful of people that have gone into remission. And then “if diagnosed early, the prognosis is very good” and “…it is vital to control pain…. Making recovery even more difficult.” RECOVERY?? You don’t recover, perhaps you can go into remission or maybe your symptoms won’t be quite as severe. We don’t know.
So pleased you enjoyed it Le Malone. Obviously it varies patient to patient, and though no statistics exist (or it would have been measurable), I do know people who’ve had remission when treated immediately/inside that 3-month window. Others who have ‘remissions’ aren’t remissions in the true sense of the word, because, as you say, it’s not a recovery. But do think you may be confusing this remission with the ebbs and flows of the disease, which even at its kindest, still involves constant, severe pain. Sadly, knowledge is so slender, and waiting lists for experts often exceed this tiny 3-month window. What works for some also doesn’t work for another with no guarantees. My own experience had a reemission of sorts, but the CRPS returned with avengence after a severe trauma a few years later, now being 16 years and systemic. The theory behind why it is reversible in these initial months is based upon the as-yet unchanged brain. Once the CRPS-indiced neuroplasticity becomes so extensive — with one study saying that the brain of a CRPS patient looking like it had been completely ripped out and rewired (perhaps more articulately! Pain brain stikes again 😉 ) — that’s why it becomes increasingly more difficult but never give up hope because, as you say, we don’t know but do our best each day we can. I hope you continue to enjoy the posts. Gentle hugs x
I found this one of the most informative articles I have ever found on the subject. I live in the UK. I developed RSD/CRPS after hand surgery 6 years ago. I will be eternally grateful to the hand therapist, who spotted what was going on, well within the 3 month window. I went into remission and have probably 75% function in my left hand.- I can play golf but have lost fine motor skills. What no one seems to be able to tell me are the long term effects and prognosis. I have just had to have further surgery, on my good hand, and have to say am extremely anxious of recurrence. Thank you for the very good info. xx
Grateful to your hand specialist too, Jill. CRPS when caught early does have a good prognosis, but given the constant intensity of the pain/other many symptoms, it’s entirely understandable that you’d be worried. Take comfort in the early prognosis but also protect yourself by taking a hefty dose of good-quality Vitamin C daily (1000mg but it’s ‘water-soluble’ so you cannot overdose on Vitamin C). The long-overdue research, growing awareness, and equally growing community is bringing hope and comfort to many. Right now the main focus for you aside from Vit C is physical therapy, calming tools for both thoughts and your CNS, and the healthy neuroplasticity, which is becoming integral to treating, and managing CRPS but do think it crucial even if you did catch the CRPS early. Wishing you continued health. Thanks for your lovely comment. ♥ x
I’ve had CRPS, type II 21 years now, however required 6 years for diagnosis. I was a nurse in the OR, ironically I’m prevented from plying my vocation to help others by a disease that cannot be surgically removed. Meanwhile needed a pacemaker, and with length of time SCS is no longer an option. I find comfort that more research is finally being done, more support groups and sites, like yours are being established. Although I’ve improved with PT and some meds, CRPS is my constant companion. Thank you for all you do and all the information you pass along. We are our own advocates and together we strengthen each other.
I love that, Lorna: ‘We are our own advocates and together we strengthen each other’ CRPS is so far beyond normal understanding, frequently so far beyond even medical understanding but we do find strength in uniting—even if housebound or stuck in bed, and that’s a wonderful thing. So sadden by how long you’ve had CRPS but your attitude is inspirational. You’ll no doubt also remember when there were so few sites (just two when I was diagnosed, and imagine even less support for you when you were finally diagnosed after 6 years). I too take comfort in the long-overdue research, awareness, and connection. Thanks for your kind comment. Gentle hug ♥ x
In my almost 2 decades of enduring this disease, may I say, this is one of the most well written articles I have seen! It is also chock full of the most excellent advice and protocols! I have been mentoring and advocating for RSD/CRPS patients since 1998, and the number 1 MOST important thing, I tell ALL people with RSD, is to find ANY way they can, to keep moving! It is refreshing to see a younger demographic realize the importance of this as well! No matter our situation , we are ALL capable of finding some way to move. AND Some way to try and remain positive,even if it is part of the time. It is vital for our physical and emotional health. Really Well written piece,with GREAT info! Looking foward to reading and exploring more of your stuff! I have been saying this for many years to other people who endure RSD- “. Dont let your RSD Define you! Instead, Choose to DEFY It!” “We have RSD but it DOESNT have us!
Mimi, so lovely to read your comment and delighted you enjoyed this post. There are a few things in it I will be expanding on but TOTALLY agree with everything you said. It can be the humblest of movements (as opposed to punishing exercise) but it’s natural to not want to move when in pain, especially when everything we learnt prior to CRPS suggests that pain means STOP! So happy to read your comment, thank you, and you’re welcome too of course. Keep defying that inner gremlin MiMi! Much love and gentle hugs x
Hello. I am living with CRPS at the moment and this article was GREAT! It got my family to understand, it’s hard! And it says it’s more excruciating than childbirth, and my mother said that’s the most excruciating pain.
Thank you Leslie, so pleased you enjoyed the post and thanks for commenting. Your family’s understanding is a blessing indeed. It’s so hard for others on the other side of the painful window that is CRPS to comprehend, especially as it’s so contrary to our usual understanding of illness and pain. Wishing you strength and healing, continued support and far less pain. ♥ x
I was wondering, where is late-stage, neurological Lyme Disease (and myriad co-infections) of the McGill Pain Scale? This is also an epidemic that is DENIED by the mainstream medical community. I wonder if our illnesses are related? Most people with Fibromyalgia, with the right testing, are shown to be in some stage of Lyme. The thing is, standard testing is about 20 to 30 % accurate. I went for over 10 years undiagnosed, so if you have this kind of pain and near involvement please make sure the root cause is being addressed. Gentle hugs to all who suffer from Chronic Illness…
Thanks for your comment Karen. I do not know about late-stage Lyme Disease on the the McGill Pain Scale specifically but do know Lyme and CRPS are not related. The symptoms of fibro and Lyme however, do so frequently overlap and I too have read a few things suggesting co-existing conditions. Thank you for the gentle hugs ♥ wishing you the same and much relief, support and strength too. x
Thank you. Thank you for this webpage and all of the information. I have been struggling with CRPS and continually put on a brave face as people just don’t understand what I am going through. And when I do try to explain, I get frustrated with people not understanding. I’ve showed this site to my boyfriend who is trying to understand my condition, but just doesn’t seem to get it. I am 28 and have lived a healthy active life, so this has significantly changed my life and removed my independence. I can’t drive, can only walk short periods and am on disability from work. I couldn’t even imagine working right now. Thank you thank you thank you for your words, your advice and your simplicity. I hope you don’t mind but I have started my own blog, as a coping mechanism to voice how I truly feel through all of this. To explain CRPS I have taken quite a bit of your material, although referenced. Please let me know if you have any concerns with this!
You’re so welcome Erin, really happy it helps you. My CRPS started very young too and think we strive all the harder to keep up with friends in their 20s but end up hiding the pain all the more, flaring up viciously afterwards, and then of course, feeling so disheartened. I don’t know how long you have had CRPS but the things that truly ring out above others for helping reemissions or even just a reduction in the symptoms are: gentle movement in warm water/aqua physiotherapy, GMI or graded motor imagery, which is part of brain retraining or the neuroplasticity aspect of pain and CRPS (a little detail above but expanding this into a post of its own). Also t’ai chi (even in a chair or some movements can be done in a bed), restorative yoga (see recent post on this). I was even more touched to read your lovely intro about this site on your blog ♥ That means so much. Keep me posted Erin. Gentlest hug ♥ x x
Thank you for this well-written thorough explanation and suggestions, no doubt gleaned by years of personal experience. I am glad you specify aggressive yet gentle. Some well meaning, physical therapists think that by aggressive, they have to push the patient through weight bearing exercises and painful desensitizing exercises. And they think if you are not screaming, you’re ok, when most CRPS patients want so much to be well they will tolerate what they can to improve. Gentle is the operative word and you stress that so well in your post. This made a HUGE difference for me. I tried all the approaches you suggested. And yes aqua therapy as a natural aid to promote compression. The GameReady Ice machine also helped restore warmth to my foot, introduced very cautiously and gradually as of course direct ice can not be tolerated by most CRPS patients. Sadly, some to that as a way to numb pain but may suffer for it later. It is important that the PT is very knowledgeable about nerves and does gentle nerve gliding (or as some say ‘nerve flossing’) exercises as well, as slow movements as you suggest. And the non affected side should always be worked at the same time. Thanks for helping others through your own painful journey. There is hope for those who are treated later, but all these approaches will aid recovery. A touch therapy called somatic experiencing was also helpful in calming the traumatized sympathetic nervous system and dipping into the parasympathetic system, along with slow breathing, warmth, and gentle movement. And yes, even if that means nothing but toe or finger wiggles at first. I never imagined I would be running 10Ks again and training for half marathons. I hope everyone who reads this site can also experience the gift of remission.
Loved reading your comment, Yvonne. It’s also filled to the brim with such useful info and tips. Thank you for sharing this, as I know others will find hope and healing in your words. Gentle, definitely. I truly wish that was known/advocated decades ago, and ice too, which truly hampered my own journey, and that of so many others with CRPS too but as you say, this site is a very silver lining from that journey, and it fills me with joy that you appreciate it, but more so, are in a remission. I did neglect to mention about exercising both sides if one is unaffected, so thank you for that. Wishing you continued healing and hugs. ♥
First of all thank you so much for your website the information you have provided is very beneficial to all suffering this condition,I have been suffering mentally and physically with CRPS since the age of 11. Mine is just in my left foot, I find it also affects
My immune system. When I was younger I used to get sick all the time and didn’t exactly know why, and my lymph nodes have always
Been swollen since having the condition. I was wanting to know if you experience the same thing as I often feel so confused about it. I have had many
Scans and blood test and doctors have said that my lymph are perfectly healthy. Unfortunately since having CRPS I have suffered from severe health anxiety
As for me it all started with a simple fracture in the growth plate and then blew out of proportion, so now I catastrophes everything. Can you please clarify for me how CRPS does affects the immune system and lymph nodes thanks xx
Hi there! Great article you have, I would also want to share my thoughts that Meditation indeed has positive effects not only in the body but also in the mind, a total holistic wellness that brings us to know our inner-self better. It gives us a peace of mind that helps us have a much better perception about our lives.
Our advocacy is to promote the positive effects of meditation, yoga and inner wellness.
Help us, visit our website at http://www.iamthechangeiseek.org and also http://www.goodreads.com/kathleensuneja or http://bookstore.xlibris.com/Products/SKU-0058696049/I-Am-The-Change-I-Seek.aspx or http://www.amazon.com/Am-Change-Seek-Primer-Realization/dp/146534778X.
You can also download the app at https://play.google.com/store/apps/details?id=com.goodbarber.iamthechange.
Thank you and have a great day!
Thank you for all this information and supportiveness – certainly needed!
Does anybody know anything about a medical, bodily-infusion treatment for CRPS which is practised in Italian hospitals and apparently curative?
I don’t think positive outlook will cut it for me, can’t see or feel ANYTHING positive about my CRPS (also sheer hell for nearest and dearest) and I definitely do not want to live with it. But I should like to have attempted a practical solution, and welcome any useful information or experiences of this.
Many thanks!
Hi Rhiannon, I’m currently researching just that so I’ll save your email and cc you on the info, and will also be adding this to the main CRPS page. Understand completely re positivity. It’s so hard when in such relentless and severe pain, much less a complex condition even doctors do not understand. You’re not alone, though I know it so often feels that way. Wishing you far kinder days and hope for all of us. Gentle hug x
Thank you for all the wonderful information I have CRPS as well as chronic back pain. The treatments from my specialist help the the CRPS but lately my leg feels so cold it keeps me awake. I have not found any references on how to deal with this part of the pain. Does anyone have any suggestions. I have tried massaging the leg, warm epsom salt baths among other things currently the pain is mostly controlled but now this I am trying to stay clear of medications if at all possible
Hi, I have suffered CRPS T1 since 1998/99. Workplace injury with the accompanying Insurance Company fighting Tooth and Nail. Court cases, “their Occupational Physicians”…. Living in a small Town and no real Medical Expertise, my Husband and I flew to our closest Main City and secures a consultation with a Sub Foot Specialist. He immediately diagnosed CRPS T1. He would not front Court though as the Government did not recognise the condition.
Many thousands out of pocket and still fighting an Insurance Company, I finally had had enough and left work. I was worse than ever and only getting Sleep when my Body demanded it and ‘took over’. It would last for perhaps 30 mins if I was lucky. Even asleep, my Husband said I thrashed , kicked and Moaned non stop.. I was finally sick of it all. Nothing was helping, not even the Doctor at the time practicing her ridiculous ‘type’ of Doctoring on me. Changed to another in the Practice, who told me to get a name of a Specialist and he would provide a Referral.
Thank goodness for Google! Gave me several names went back to Doctor and he had heard of the first who had a good reputation…. The Specialist flew into a major City 3 hours from our home. We drove up to see him several times, (at a high cost)..
That Man who is a Neurosurgeon from Melbourne is my Hero. He implanted a Pulse Generator in my Spine cutting off that terrible Pain signal. As it was a Trial Surgery, with the Government not recognising the condition, I had to pay for everything myself. Every Cent has been worth it! Yes there are times I can still feel a bit of pain but it is very minor to what I experienced in the past. He gave me back a Life.
Shame on Insurance Companies and their Occupational Physicians and Thank you to a man I have great respect for, Mr Richard Sullivan.. Melbourne Australia. Jill
This is why there is a prevention month of pain syndrome because most of us ignore this issues but it mustn’t. I am happy to have this regional pain syndrome advocacy.